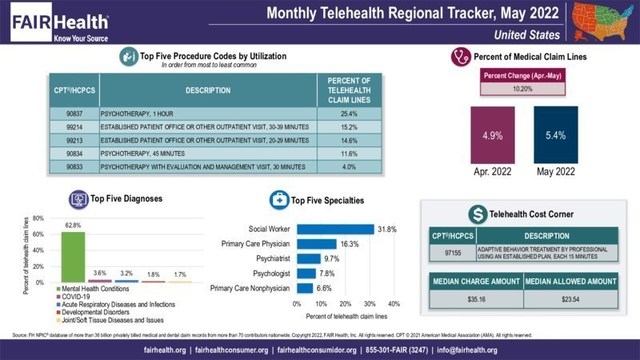
In May 2022, for the second straight month, telehealth utilization, as measured by telehealth’s share of all medical claim lines, grew nationally and in every US census region (Midwest, Northeast, South, West), according to FAIR Health’s Monthly Telehealth Regional Tracker.1 National telehealth utilization increased 10.2 percent, from 4.9 percent of medical claim lines in April to 5.4 percent in May. Regionally, the greatest increase was in the Midwest, where telehealth utilization grew 17.6 percent in May. The data represent the privately insured population, including Medicare Advantage and excluding Medicare Fee-for-Service and Medicaid.
The rise in telehealth utilization in May could have been due to the growth in the number of COVID-19 cases as reported by the Centers for Disease Control and Prevention. The increased risk of infection may have led more patients to avoid in-person care.
Diagnoses
From April to May 2022, COVID-19 climbed in the rankings of the top five telehealth diagnoses nationally and in every region except the Northeast, where it remained at number two. Nationally, COVID-19 rose from third to second place; in the Midwest, from fourth to second place; in the South, from unranked to third place; and in the West, from fifth to second place.
In the South, three diagnoses fell out of the top five telehealth diagnoses from April to May. They were encounter for examination, hypertension and developmental disorders, replaced, respectively, by COVID-19, skin infections and issues, and urinary tract infections.
Specialties
From April to May 2022, in the Midwest, psychiatrist dropped from fourth to fifth place in the list of top five telehealth specialties, switching places with primary care nonphysician.
Procedure Codes
In May 2022, the rankings of the top five telehealth procedure codes did not change nationally or in any region when compared to the prior three months. The number one telehealth procedure code nationally and in every region remained CPT®2 90837, one-hour psychotherapy.
Costs
For May 2022, the Telehealth Cost Corner spotlighted the cost of CPT 97155, adaptive behavior treatment by professional using an established plan, each 15 minutes. Nationally, the median charge amount for this service when rendered via telehealth was $35.16, and the median allowed amount was $23.54.3
About the Monthly Telehealth Regional Tracker
Launched in May 2020 as a free service, the Monthly Telehealth Regional Tracker uses FAIR Health data to track how telehealth is evolving from month to month. An interactive map of the four US census regions allows the user to view an infographic on telehealth in a specific month in the nation as a whole or in individual regions. Each infographic shows month-to-month changes in telehealth’s percentage of medical claim lines, as well as that month’s top five telehealth procedure codes, diagnoses and specialties. Additionally, in the Telehealth Cost Corner, a specific telehealth procedure code is featured, with its median charge amount and median allowed amount.
FAIR Health President Robin Gelburd stated: “We welcome sharing these varying windows into telehealth utilization as it continues to evolve. This is one of the many ways we pursue our healthcare transparency mission.”